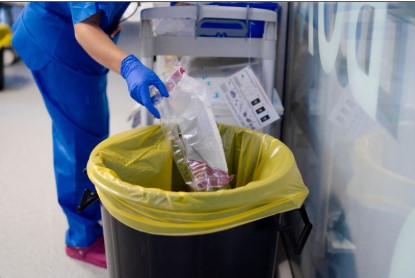
Proper medical waste disposal is essential for maintaining a safe and compliant healthcare environment. Hospitals, clinics, dental offices, and laboratories generate various types of regulated medical waste, including sharps, contaminated materials, and pathological byproducts, all of which pose potential health risks if mishandled. Medical waste disposal in Virginia ensures responsible disposal protects staff, patients, and the community while safeguarding the environment from contamination. By following best practices, healthcare providers can reduce exposure risks, comply with Virginia DEQ and federal regulations, and prevent costly fines or operational interruptions. Understanding the protocols for classification, segregation, storage, transport, and treatment is key to effective medical waste management.
What Is Medical Waste?
Medical waste refers to byproducts generated during healthcare activities that may pose risks of infection or injury. Common categories include sharps (needles, lancets), pathological waste (tissues, body parts), and contaminated materials such as gloves, gowns, and dressings. Unlike general waste, medical waste requires careful handling due to its potential to transmit disease or cause harm if mismanaged.
In Virginia, medical waste is regulated under the Virginia Department of Environmental Quality (DEQ) and federal guidelines. Adhering to these standards ensures environmental protection, public safety, and compliance with state and federal laws.
Regulatory Framework
Compliance is central to medical waste disposal in Virginia. Healthcare facilities must comply with regulations governing classification, storage, transport, treatment, and final disposal. Key regulatory frameworks include:
- Federal Standards: The Resource Conservation and Recovery Act (RCRA) governs the management of hazardous and regulated wastes, including some medical waste categories.
- State Requirements: Virginia DEQ mandates labeling, containment, and the use of approved treatment methods for medical waste. Facilities must maintain records of handling and disposal practices.
Non-compliance can lead to fines, reputational damage, and legal issues, making adherence essential for healthcare operations.
Segregation and Handling Best Practices
Effective disposal begins with proper segregation at the point of generation. Best practices include:
- Separate Waste Streams: Sharps should go in puncture-resistant containers, while biohazardous materials are stored in red biohazard bags.
- Containment: Containers must be sturdy, leak-proof, and labeled clearly to prevent exposure.
- Minimize Contamination: Avoid overfilling containers and clean up spills immediately with approved disinfectants.
These steps reduce occupational exposure risks and simplify processing for transport and treatment.
Storage and Transportation
After segregation, medical waste must be stored securely. Virginia regulations require designated storage areas that prevent public access, control temperature, and limit accumulation time. Transportation must be handled by licensed waste carriers complying with Department of Transportation rules. Professional providers like Secure Waste Systems ensure waste is transported safely to treatment facilities in accordance with all regulations.
Treatment and Final Disposal
Treatment methods render medical waste non-infectious before final disposal. Common options include:
- Autoclaving: Steam sterilization to destroy pathogens.
- Incineration: High-temperature combustion for pathological or pharmaceutical waste.
- Microwave Treatment: Disinfection using microwave energy.
Treated waste can then be disposed of in licensed landfills. Choosing a qualified disposal partner ensures compliance with all legal and environmental requirements.
Staff Training and Documentation
Training staff on proper handling, segregation, and emergency protocols is essential for safe operations. Facilities should maintain accessible written procedures, reviewed regularly for updates. Documentation of manifests, treatment certificates, and training logs ensures compliance during inspections and audits.
Conclusion
Implementing best practices for medical waste disposal in Virginia requires a comprehensive approach from proper segregation and storage to treatment, transport, and meticulous record-keeping. Partnering with experienced service providers ensures compliance, enhances safety, and reduces operational risks. Well-trained staff, effective processes, and robust documentation create a safe and efficient waste management system. For healthcare organizations, professional services often include additional offerings such as hazardous waste pickup, streamlining disposal, and ensuring full regulatory compliance. Following these practices helps facilities maintain a safe environment while meeting all state and federal requirements.